
Hydrogen (H 2) and methane (CH 4) are exclusively produced by microbial metabolism and are exhaled on the breath ( 6– 8). Alternatively, a breath test can be used to assess microbial overgrowth in the gut. Also, there may be sampling errors given that only a small segment of the small bowel can be aspirated, leaving the rest unexplored. However, aspiration is invasive and expensive, requiring a skilled gastroenterologist. 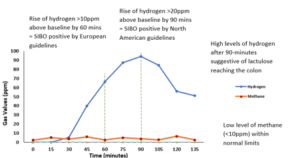
While a diagnosis of IBS is based on clinical symptoms, the gold standard for a diagnosis of SIBO is the presence of ≥10 3 colony forming units per milliliter (CFU/mL) of jejunal aspirate by culture ( 4, 5). One manifestation of dysbiosis, small intestinal bacterial overgrowth (SIBO), is linked to IBS and will be the focus of this review. The last category, the gut microbiome, has seen an exponential growth in interest over the last few years. 
The complex network of etiologies likely represents various pathophysiological states that may be unique to the patient and include visceral hyperalgesia, intestinal permeability, immune activation, altered gastrointestinal motility, autoimmunity, and alteration of the gut microbiome. Although these treatments can be effective, newer studies have demonstrated more complex, organic etiologies specific to the gut that have led to novel therapeutic options. Because of this, many treatments focus on antidepressants and neurobehavioral intervention ( 3). Historically, IBS has been associated with stress and anxiety, and the brain-gut axis has been widely described as important in understanding IBS ( 2). Patients may experience various comorbidities including, but not limited to, bloating, constipation, diarrhea, incontinence, and psychological disturbances. Symptom onset must occur at least 6 months prior to diagnosis, but many patients suffer long-term chronic symptoms as a result of this disorder. Irritable bowel syndrome (IBS) is a functional bowel disorder defined by recurrent abdominal pain for at least 1 day per week in the last 3 months that is associated with 2 or more of the following: related to defecation, associated with a change in stool form, or associated with a change in stool frequency ( 1). This review will focus on the role of the gut microbiome and SIBO in IBS, as well as novel innovations that may help better characterize intestinal overgrowth and microbial dysbiosis. Furthermore, gut microbiome dysbiosis may be associated with select neuropsychological symptoms, although more research is needed to confirm this connection. As a consequence, SIBO and IBS share a myriad of symptoms including abdominal pain, distention, diarrhea, and bloating. Due to gut microbiome dysbiosis, patients with IBS may have increased intestinal permeability, dysmotility, chronic inflammation, autoimmunity, decreased absorption of bile salts, and even altered enteral and central neuronal activity. smithii is an archaeon and can overgrow in areas outside of the small intestine, it was recently proposed that the term intestinal methanogen overgrowth (IMO) is more appropriate for the overgrowth of these organisms. In addition, Methanobrevibacter smithii, the causal organism in a positive methane breath test, has been linked to constipation predominant irritable bowel syndrome (IBS-C). Numerous pathogenic organisms have been shown to be increased in subjects with SIBO and IBS, including but not limited to Enterococcus, Escherichia coli, and Klebsiella. SIBO can be diagnosed either by a small bowel aspirate culture showing ≥10 3 colony-forming units (CFU) per mL of aspirate, or a positive hydrogen lactulose or glucose breath test. Small intestinal bacterial overgrowth (SIBO) is one manifestation of gut microbiome dysbiosis and is highly prevalent in IBS (Irritable Bowel Syndrome).
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
